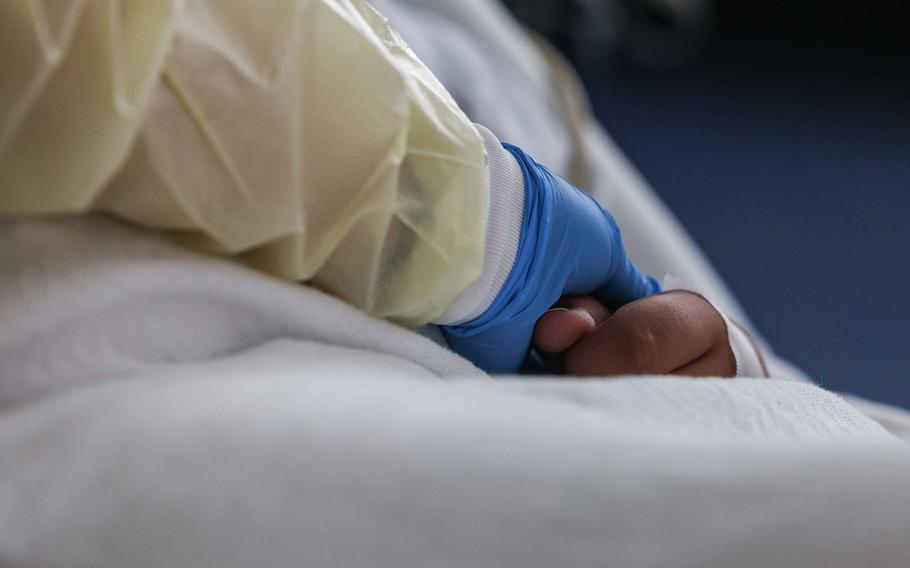
Nurse Christina Walker checks on Francisco Rosales, 9, who is being treated as a COVID-19 patient in the pediatric intensive care unit at the Children’s Medical Center in Dallas on Aug. 13, 2021. (Lola Gomez/Dallas Morning News/TNS)
Stars and Stripes is making stories on the coronavirus pandemic available free of charge. See more stories here. Sign up for our daily coronavirus newsletter here. Please support our journalism with a subscription.
DALLAS (Tribune News Service) — The last 23 months have been the hardest of Gabriela Whitener’s 27-year career.
For almost two years, the North Texas nurse has fought on the frontlines of the war against the coronavirus.
That’s two years of watching her patients struggle to breathe. Two years of serving as a family member for patients taking their last breath alone in a COVID-19 ward. Two years of worrying about younger nurses who have only ever worked in a post-COVID world.
As the highly-contagious omicron variant sweeps through Dallas-Fort Worth, threatening once again to overwhelm hospitals and already-exhausted health care staff, Whitener and her colleagues are prepping for yet another damaging battle.
“Have you ever watched those movies of when the army is in the trenches and they pray before the fight? We as a unit, as nurses, we always pray before the shift starts,” said Whitener, who is also a clinical assistant professor at the University of Texas at Arlington.
At the beginning of the pandemic, health experts knew it would be a long road to recovery. A marathon, not a sprint. Two years later, nurses and other frontline workers are running their fourth marathon, and the finish line is nowhere in sight.
Health care staffing shortages aren’t helping. Even Thursday’s announcement of 1,000 traveling nurses anticipated to arrive in North Texas over the next week likely won’t be enough to fill gaps in staffing.
The toll COVID-19 has put on nurses likely won’t be felt in full for months or years. But, already, the pandemic’s most important line of defense is showing troubling signs of severe trauma.
“I think we’re already seeing [post-traumatic stress disorder],” said Barbara Chapman, nurse practitioner and University of Texas at Tyler clinical assistant professor. UT Tyler’s generic bachelor of science in nursing program admits 160 students per semester, according to the university’s website.
Advocacy organization Mental Health America said 93% of health care workers surveyed last year were experiencing stress and 86% reported anxiety. Three-fourths said they were overwhelmed.
Nurses were less likely to have adequate emotional support than other health care workers, the survey also found.
“I used to say these folks are overwhelmed, but they’re past overwhelmed,” Chapman said.
Perhaps most concerning is the experience of “moral distress” – questioning one’s purpose in life or work.
“That differs from things like fatigue and burnout, because it’s really about questioning if what you’re doing is the right thing,” said Meagan Rogers, associate chair of undergraduate nursing at the University of Texas at Arlington. The university is the largest producer of baccalaureate educated nurses in the state.
Even among nurses who frequently witnessed death before the pandemic, COVID-19 brought unprecedented levels of patients dying. “They’re seeing more death, there’s less they’re able to do,” she said.
More than 827,000 people in the U.S. have died from COVID-19 since the start of the pandemic, according to data from the Centers for Disease Control and Prevention. In Texas, that number is nearly 75,000.
“As a nurse, you’re trained to take care of people, to help them recover and to get them back home to their environment, to their families,” Whitener said. “We were not able to recover as many patients as we would have wanted and that brings a sense of, for lack of a better word, failure.”
Whitener and the nurses she trains serve as far more than just the people responsible for a patient’s physical wellbeing.
And while taking on the role of caretaker, therapist and friend for patients is nothing new in the nursing profession, limitations on hospital visitors during pandemic peaks blurred the lines of professional responsibilities and personal care.
“Let’s say I’ve had a day or two off, and when I get back I check on my previous assignments to see how my other patients were doing,” Whitener said. “We get attached to our patients, it’s in our being to be like that.”
Record numbers of nurses and other health care workers have left the field entirely because of the pandemic. Between February 2020 and October 2021, 18% of health care workers quit their jobs, according to a survey by data intelligence company Morning Consult. Of the workers who stayed, 31% have considered leaving.
The national worker shortage is stressing hospital systems and forcing already burned-out health care workers to take on even larger case loads. Omicron is also infecting more health care workers than any other variant, worsening the strain on staffing.
In an effort to combat the pandemic’s effect on health care workers and students, medical and educational institutions are creating spaces for discussion about the difficulties of treating COVID-19 patients.
UT Tyler, for instance, has set up a free mental health care outreach line to help connect educators and health care workers with additional resources.
Nursing students at UT Arlington have lessons on burnout, self care and compassion fatigue integrated into their curriculum. The university recently added a course on the transition from school to work to help ease the transition into full-time nursing.
But, for the most part, nurses and other frontline workers have had to find their own coping strategies to handle the stress of their jobs.
For Whitener, that means leaving her work at the hospital as much as possible. She and her son, who is also a nurse, try not to talk about their jobs while at home.
“Home is my sanctuary, and I like to recover at home, so I just don’t want to bring work [there],” she said.
She’s made her life as simple as possible. She cut her hair because it was easier to keep under a cap during 12-hour shifts. While she used to make sure her makeup and nails were always done, she now focuses her mornings on preparing her personal protective equipment.
When she gets home from a long day, Whitener said she looks forward to taking care of her two dogs and her own physical health through exercise. She makes time for the little things, like taking a hot bath with relaxing salts.
The pandemic, Whitener said, has given her a different perspective on life.
“It made me pay attention to what matters most,” she said. “And at some point I realized that I matter a lot.”
____
©2022 The Dallas Morning News.
Distributed by Tribune Content Agency, LLC.