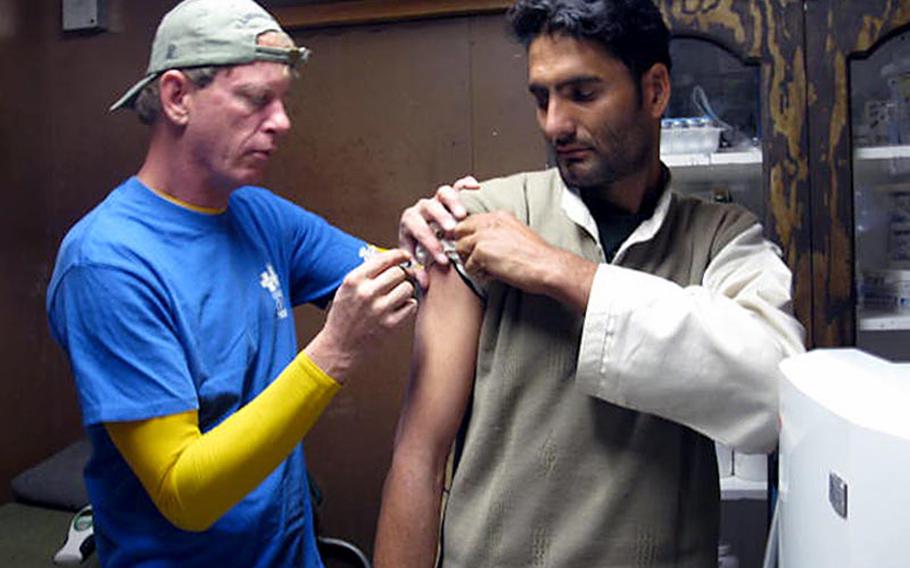
Civilian medic Cory Kraus gives Abdul Aman Hijartullah one of several rabies shots after the Afghan, who works for a subcontractor hauling trash from FOB Apache to the dump, was bitten by a dog and feared he'd get the deadly disease. (Courtesy Cory Kraus)
HEIDELBERG, Germany -- An Indian escort, a group of American medics, the U.S. military and fear itself helped an Afghan trash hauler avoid a possible death sentence from rabies recently, just a few months after an American soldier infected with the disease died.
For the Afghan, infection normally would have meant death, but the awareness created by the unusual death of the soldier may have helped save his life.
Cory Kraus, the sole medic at Forward Operating Base Apache, knew that the trash hauler, Abdul Aman Hijartullah, needed preventive rabies treatment as soon as he saw the wound on the man’s leg and heard that he had been attacked by a dog. Kraus’ awareness of the lethality of rabies, like that of most medical providers in the country, had been raised four months earlier by the rabies death of the U.S. soldier bitten by a dog while deployed in Afghanistan.
Further, part of the recommended postexposure treatment, a delicate, costly medicine called human rabies immune globulin, “is in short supply and available mainly in industrialized countries,” according to WHO. It is almost impossible to get in Afghanistan.
“If an Afghan gets rabies, they generally die,” said Mark Caplin, a physician’s assistant in Kandahar working for Onsite OHS, a company that contracts with Dyncorp International to provide health care to its workers.
Kraus, who also works for Insite OHS, didn’t want that for Hijartullah, 26, and the father of two.
“I don’t want anyone to die of rabies,” Kraus said in an email.
Spc. Kevin Shumaker’s death in August sparked an investigation into why the soldier died of a disease that’s preventable if postexposure treatment is given but is almost always fatal without treatment.
The investigation found that Shumaker, a cook with the 615th Military Police Company, did not report his dog bite to his command or seek medical attention.
But it also found that his command had been remiss and cited a “concerning lack of knowledge” about rabies by some U.S. military medical personnel, most of whom had never seen a rabies case. Dogs and cats in the United States are vaccinated against the virus; in the extremely rare human cases in the U.S., the usual cause is a bat bite.
By contrast, four of 35 dog heads sent in a year from Afghanistan for rabies testing at the Army veterinary lab at Landstuhl, tested positive, the investigation found.
After Shumaker died, according to Lt. Col. Steven Cersovsky, senior epidemiologist at the Army Public Health Command, “both in theater and in the States, awareness went up.”
Hijartullah, though, already knew the key fact about dog bites and rabies. Eight years earlier, his village imam had been bitten by a dog and died a terrible death from the rabies virus.
“It causes agitation, terror and convulsions,” wrote Dr. Rodney Willoughby Jr., a rabies expert in Scientific American Magazine in 2007.
“Victims suffer painful throat spasms when they try to drink or eat. Paralysis follows, yet people infected with rabies are intermittently alert until near death and can communicate their fear and suffering to family and caregivers.”
Hijartullah washed his leg after the dog bit him and put salt in the wound. He went to the local bazaar seeking a better treatment and was told there wasn’t any.
“They told him not to worry about it,” Kraus said.
But Hijartullah did worry, and the next morning when he reported to FOB Apache, he discussed his worries with his on-base escort, Raveendran Kizhu Veetil. U.S. bases assign escorts to Afghans when they’re on base as a security measure. Veetil, from India, which also has a high rate of rabies, also was frightened. He urged the Afghan with whom he conversed in Urdu, to seek help from the Americans.
Veetil accompanied Hijartullah to the U.S. security people in charge of them, then provided crucial English translation.
Before long, both of the men were at Kraus’ clinic.
Kraus called his boss, physician assistant Bill Weiss, based at FOB Tarin-Kowt. Weiss ordered a tetanus shot, an antibiotic and the series of Rabivert rabies vaccine, all easily available.
But there was still a problem.
“We realized that there was no available HRIG” — human rabies immune globulin — Weiss wrote in an email. “This is a critical part of the protocol for folks not previously vaccinated with anti-rabies medicine,” he said, such as military dog handlers and veterinarians.
HRIG provides more immediate protection than the vaccine. But it’s a costly medicine — about $1,200 a dose — and must be kept refrigerated. It is kept only at a few medical facilities in Afghanistan.
After phoning around, Weiss eventually learned that he could get the HRIG from the hospital on Kandahar Air Field but only if the U.S. military personnel there would give it to him.
The U.S. is obligated to provide medical care to Afghans to save “life, limb or eyesight.”
“This was kind of a gray area,” Weiss said.
Weiss then called on the persuasive talents of a colleague in Kandahar: Mark Caplin, who manages OHS Onsite medics in the Kandahar region, who made the necessary connections.
“It took about a half a day,” Caplin said in an email. “It took a lot of people doing their jobs and a little bit of paperwork.”
The effort, Weiss said, was “truly an impressive example of civilian-military cooperation” that very likely saved the Afghan’s life.
“Would this response have occurred without the death of Shumaker and the subsequent increased awareness of rabies and animal bites?” Weiss asked. “Hard to say. I strongly suspect that it did play a major factor.”