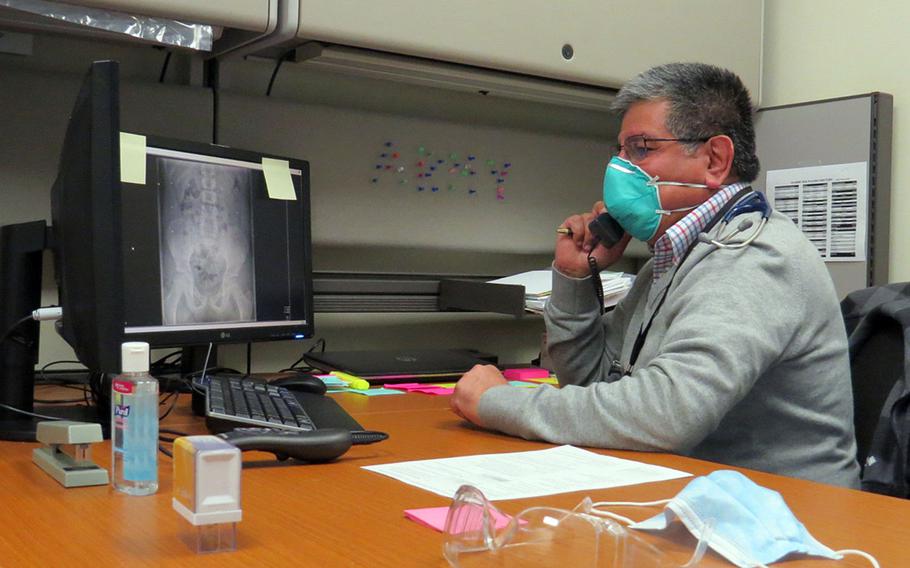
Dr. Rafael Nunez, a pediatrician at the U.S. Army Health Center in Vicenza, Italy, speaks on the phone March 9, 2021, with a parent about their child's diagnosis. Virtual appointments have been routine during the coronavirus pandemic. (U.S. Army Health Center Vicenza )
Stars and Stripes is making stories on the coronavirus pandemic available free of charge. See more staff and wire stories here. Sign up for our daily coronavirus newsletter here. Please support our journalism with a subscription.
The U.S. military has seen a surge in the use of virtual medical care, as patients avoid doctor’s offices and health care workers work to minimize their exposure to the coronavirus.
The Defense Health Agency long planned to expand its use of telemedicine, which could include everything from a nurse displaying an X-ray of a soldier’s broken foot and discussing rehabilitation, to doctors in different countries diagnosing cancer.
“We basically in a couple of months had a growth in what we were planning to do in a couple of years,” said Jamie Adler, lead for the Defense Health Agency’s Virtual Health Clinical Integration Office. “With patients and many providers at home, we really had to step up.”
Health caregivers across the military have found that many appointments can be done just as well and more conveniently using technology as simple as a cellphone.
Need a child’s rash seen to? “The parent sends us pictures, then we can make the diagnosis and talk to them,” said Dr. Rafael Nunez, of U.S. Army Health Center Vicenza. The clinic this week limited the number of patients allowed inside as Italy’s coronavirus cases spiked and most of the country again locked down.
Patients like virtual care because it’s discreet and convenient, said Col. Andrew Baxter, Regional Health Command Europe nurse executive.
Doctors like it because it’s efficient, allows for more collaboration and provides more timely appointments and access to health care. Commanders like it because it saves travel costs and mission days.
In a way, virtual health care is a back-to-the-future endeavor, Baxter said. “It’s kind of going back in time to the house call.”
The U.S. military in Europe had a five-year head start adapting virtual care because of the dispersal of troops under its responsibility. Its clinics provide primary care to operational troops deployed to Europe, Africa, Afghanistan and the Middle East.
“We have small groups of soldiers throughout Europe, sometimes in the middle of a field,” Baxter said.
The region’s telemedicine calls swelled from 7,000 in 2019 to more than 20,000 over the past year, Baxter said.
Among them was a surgical dressing change performed by a medic in remote Bulgaria as a surgeon in Germany instructed. In another case, troops in Ukraine resolved behavioral health issues with an Army provider in Poland.
Behavioral health is especially suited to virtual sessions, Baxter said. Troops with anxiety, depression, PTSD or other problems are known to dislike being seen seeking help. A virtual visit may draw no more attention than a phone call.
Complex physical ailments can also be addressed.
Endocrinologist Maj. Harris Baloch, a specialist in glandular disorders like diabetes and hypothyroidism, prefers seeing patients in person for a first appointment and physical exam at Landstuhl Regional Medical Center, the largest U.S. military hospital in Europe. After that, he sees them primarily through secure video.
Baloch also confers frequently with other physicians that way. A recent video conference to discuss an England-based Lakenheath Air Base patient’s case and devise testing and treatment included her Lakenheath doctor, a kidney specialist at Naval Medical Center Portsmouth, Va., and Baloch.
“It prevented the evacuation of the patient,” Baloch said.
For a few months last year when Landstuhl had no oncologist, a Walter Reed National Military Medical Center doctor filled the gap.
“Even Landstuhl might not have the specialty a patient needs,” Baxter said. “This brings us global reach.”
Virtual medicine had grown more slowly in the continental U.S. than in Europe until now, Adler said.
“The need wasn’t staring them in the face” until the pandemic happened, he said.
Along with the increased use came new guidance on how to use the technology safely, confidentially and effectively. Additional Defense Department security requirements were developed to safeguard appointments, Adler said.
Although most telemedicine uses phones and video, other applications have emerged. In December, some clinics began to continuously monitor COVID-19 patients’ blood oxygen levels at home.
“One of the big advantages of virtual health care is it can and does reduce the need to use more complex services,” he said. “If you can consult, you can avoid a visit to the emergency room.”
However, there will always be a place for doctors and nurses to interact in person.
“If you have the resources and the specialists or you’re there for a physical exam it makes sense to deliver it in person,” Adler said. “I think there’ll be a balance.
“But it’ll be a new balance. We’ve discovered we can do things we didn’t know we could do. And if you can talk to a mental health provider or a primary care physician in the privacy and comfort of your home ... I think patients are going to insist we continue to do this.”